2025-03-31 15:01:06
We sometimes say that cancer is like a seed buried in a person’s body for years or even decades. This seed may grow slowly or rapidly under various environmental influences until it takes root and is detected in different ways. Generally, the older a person gets, the higher the probability that this "seed" will sprout. With China's economic development, rising living standards, and increasing life expectancy, health conditions that were rare decades ago have now become more prevalent.

The Increasingly Diverse Diet of Chinese People
"Diseases of Affluence" (Modern Civilization Diseases)
Often referred to as "diseases of affluence" or "modern civilization diseases," these are non-communicable epidemics that emerge as societies become wealthier. Improved diets, coupled with reduced physical activity, lead to conditions such as:
- Constipation
- Obesity
- Colorectal cancer
- Hyperlipidemia
- Atherosclerosis
- Coronary heart disease
- Diabetes
- Stroke
Among these, colorectal cancer (CRC) and endometrial cancer (EC) are prominent members—and both are frequently linked to a hereditary condition called Lynch syndrome.
Lynch Syndrome (Hereditary Nonpolyposis Colorectal Cancer, HNPCC)
Lynch syndrome, also known as hereditary nonpolyposis colorectal cancer (HNPCC), is an autosomal dominant genetic disorder. It was first observed in 1895 by Dr. Warthin, who noted that his tailor’s family had multiple members dying from cancers—primarily CRC, gastric cancer, and EC. Later, in 1962, Dr. Henry Lynch encountered a similar family, and further cases were identified, gradually unraveling the mystery of this syndrome.
After years of research, scientists discovered that Lynch syndrome is primarily associated with mutations in five genes:
- MLH1 (15–40%)
- MSH2 (20–40%)
- MSH6 (12–35%)
- PMS2 (5–25%)
- EPCAM (<10%)
These genes belong to the mismatch repair (MMR) pathway, with MLH1 and MSH2 accounting for ~80% of cases. When these genes carry pathogenic mutations, they lead to deficient MMR (dMMR), increasing cancer risk. Since these mutations are germline (inherited), affected individuals carry the defect from birth, often leading to earlier-onset cancers.

Dr. Warthin
Prevalence and Diagnostic Criteria in China
- 2–3% of CRC patients and ~5% of EC patients have Lynch syndrome.
- According to the "Chinese Expert Consensus on the Clinical Diagnosis and Family Management of Hereditary Colorectal Cancer," the diagnostic criteria include:
- Family history: ≥2 pathologically confirmed CRC cases in first-degree relatives (parent-child or siblings).
- Additional criteria (any one of the following):
- ≥1 case of multiple CRCs (including adenomas)
- ≥1 case with diagnosis before age 50
- ≥1 case of Lynch-related extracolonic cancers (gastric, endometrial, small intestine, urothelial/renal, ovarian, or hepatobiliary cancers).
Patients meeting these criteria should undergo genetic testing.
Testing Methods
- MMR Immunohistochemistry (IHC): Detects protein expression of MLH1, MSH2, MSH6, and PMS2. Loss of any protein indicates dMMR.
- Microsatellite Instability (MSI) Testing: Detects MSI-high (MSI-H), strongly suggesting dMMR.
For dMMR patients, further germline mutation testing (blood or normal tissue DNA) is recommended for MLH1, MSH2, MSH6, PMS2, and EPCAM.
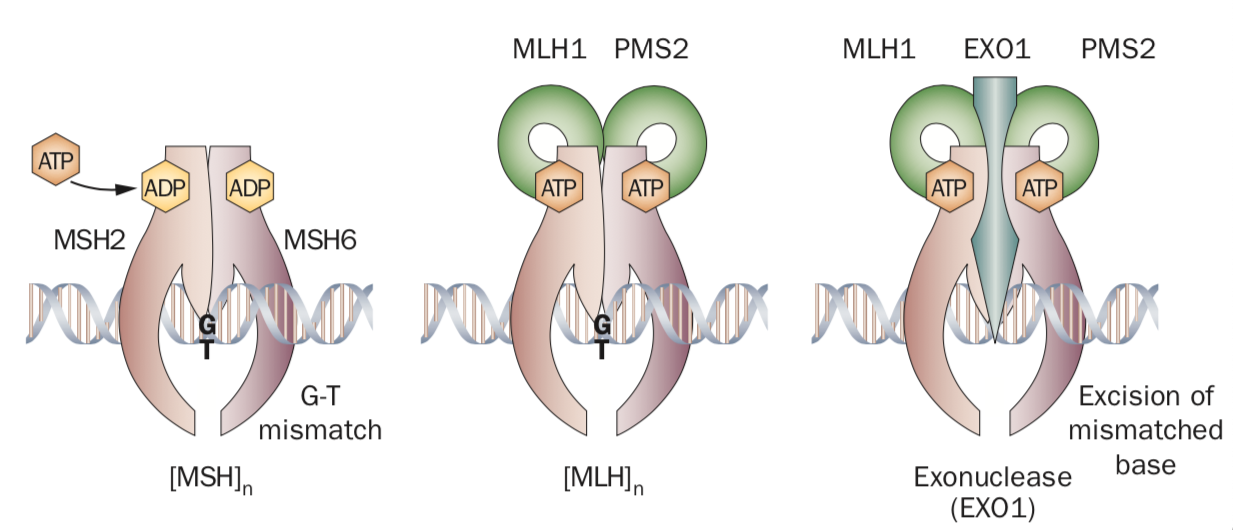
Key Players in the DNA Mismatch Repair System
The Challenge: MLH1 Methylation vs. Germline Mutations
- Some MLH1 protein loss is due to promoter methylation (epigenetic silencing), which is sporadic (non-hereditary).
- ~50% of MLH1-deficient cases are methylation-related, leading to misdiagnosis of Lynch syndrome if methylation testing is skipped.
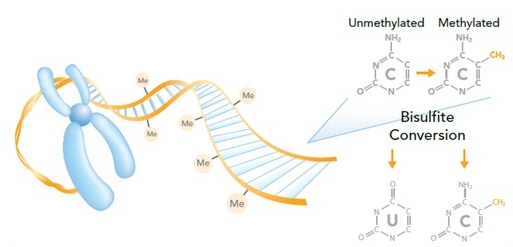
DNA Methylation
DNA methylation involves adding a methyl group to cytosine (C) at CpG dinucleotides, often in gene promoters. MLH1 promoter methylation silences the gene, mimicking a germline mutation.
Clinical Gaps and Solutions
- Many labs rely only on IHC or NGS, skipping methylation testing due to cost and workflow constraints.
- Current MLH1 methylation tests (Sanger, qPCR, ddPCR) vary in sensitivity but reduce false positives.
- Hospitals should follow guidelines strictly, combining IHC, PCR, and NGS to distinguish germline vs. sporadic cases.
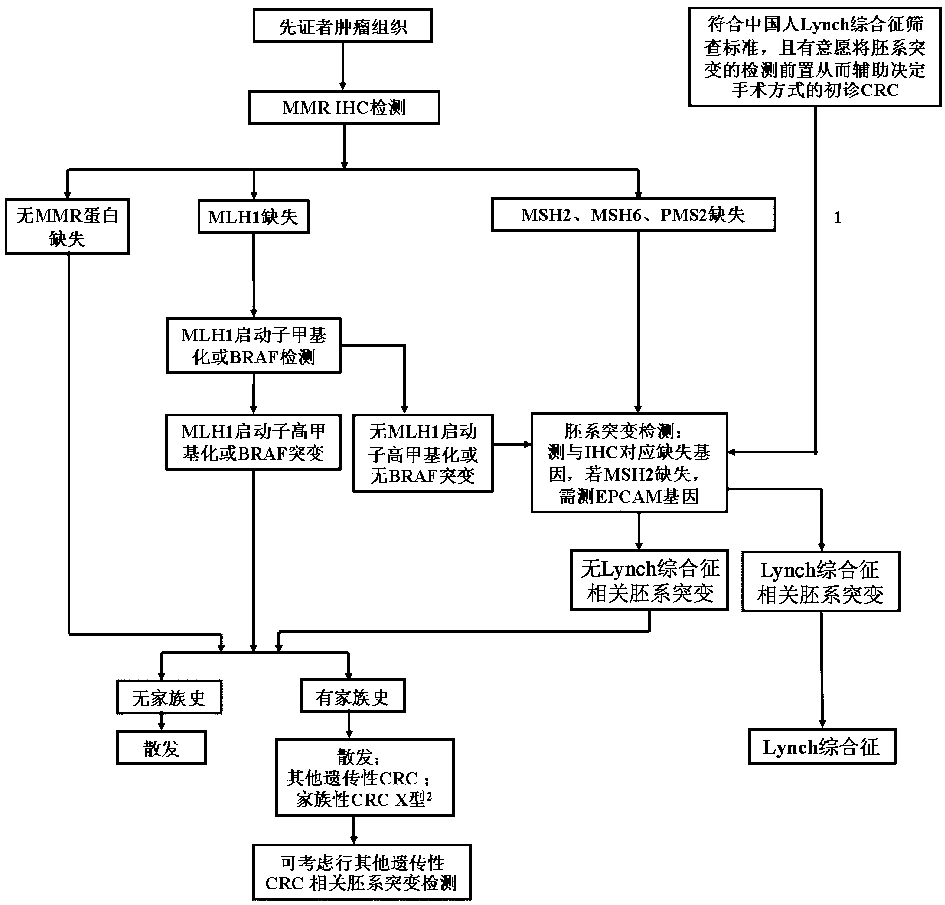
MMR IHC Screening for Lynch Syndrome in CRC
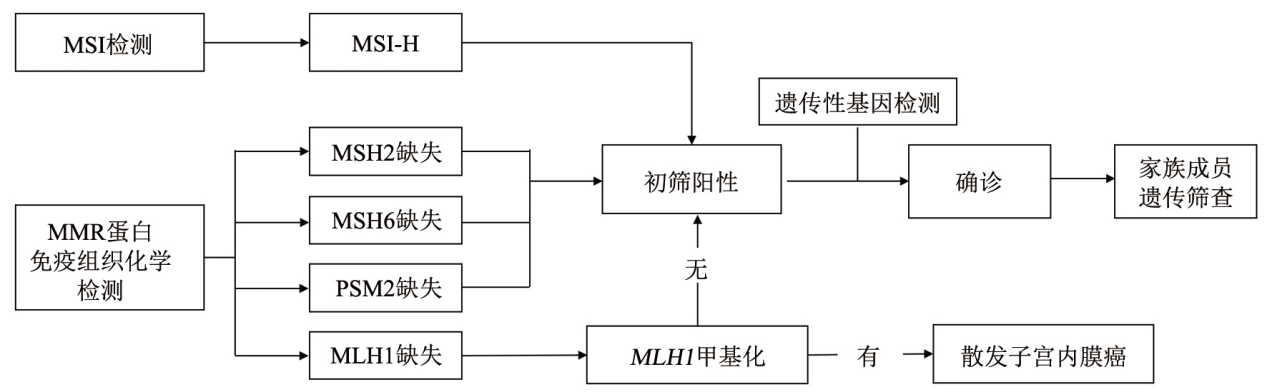
MMR/MSI Testing for Lynch Syndrome in Endometrial Cancer
Conclusion
While ideal workflows include methylation testing, real-world practices often omit it, risking misdiagnosis. Given China’s large population, improving testing accuracy is crucial to avoid unnecessary anxiety for patients and families.




